 
Regarding safety, data reported with nivolumab proved to be consistent with previously reported data with the agent in patients with solid tumors. The NUTRFS in the PD-L1–positive subgroup was not reached vs 10.9 months in the investigative and control arms, respectively (HR, 0.54 95% CI, 0.38-0.77). Specifically, the NUTRFS in the ITT population was 24.6 months with adjuvant nivolumab vs 13.7 months with placebo (HR, 0.72 95% CI, 0.58-0.89). Nivolumab was also found to improve the median non–urothelial tract recurrence-free survival (NUTRFS) and distant metastasis-free survival in both the ITT and PD-L1–positive patient populations. Approximately 40% of patients in both arms had PD-L1 positivity and 43% previously received cisplatin-based neoadjuvant chemotherapy.Īdditional results from a subgroup analysis of the ITT population indicated no differences with regard to age, sex, region, or performance status with regard to DFS benefit achieved with adjuvant nivolumab. Among those given placebo, 78.9% had the tumor of origin be urinary bladder, while 21.1% had upper tract disease. The most common reason for discontinuation was recurrent disease.Īmong those who received adjuvant nivolumab, 79% had the tumor of origin be urinary bladder carcinoma, while 21% had upper tract disease. Moreover, 53.3% of those in the investigative arm discontinued treatment vs 56.3% of those in the control arm. The median follow-up was 20.9 months for the immunotherapy and 19.5 months for placebo. 
The primary end point of the trial was DFS in the ITT population, as well as in those with a PD-L1 expression of 1% or higher. To be eligible for enrollment, patients had to undergo radical surgery within 120 days with or without neoadjuvant cisplatin or they had to be ineligible for or have declined cisplatin-based chemotherapy they also needed to be disease free per imaging. A total of 709 patients were randomized in a 1:1 fashion to receive either nivolumab at 240 mg once every 2 weeks (n = 353) or placebo (n = 356) for up to 1 year of adjuvant treatment. In the double-blind CheckMate-274 trial, investigators examined the efficacy and safety of adjuvant nivolumab compared with placebo in patients with high-risk MIUC following radical surgery. “In the CheckMate-274 trial, significantly reduced the risk of cancer recurrence or death, showing its potential to help address the need for safe and effective treatment options for this patient population.” “Even patients who appear disease free after radical surgery for MIUC are at a high risk for recurrence, with around half of patients having their cancer return,” Dana Walker, MD, MSCE, vice president, development program lead, genitourinary cancers, at Bristol Myers Squibb, stated in the press release. The median DFS with adjuvant nivolumab had not yet been reached vs 10.8 months with placebo (HR, 0.53 98.87% CI, 0.34-0.84 P <.001). The immunotherapy also improved DFS in the subset of patients with PD-L1 positivity. 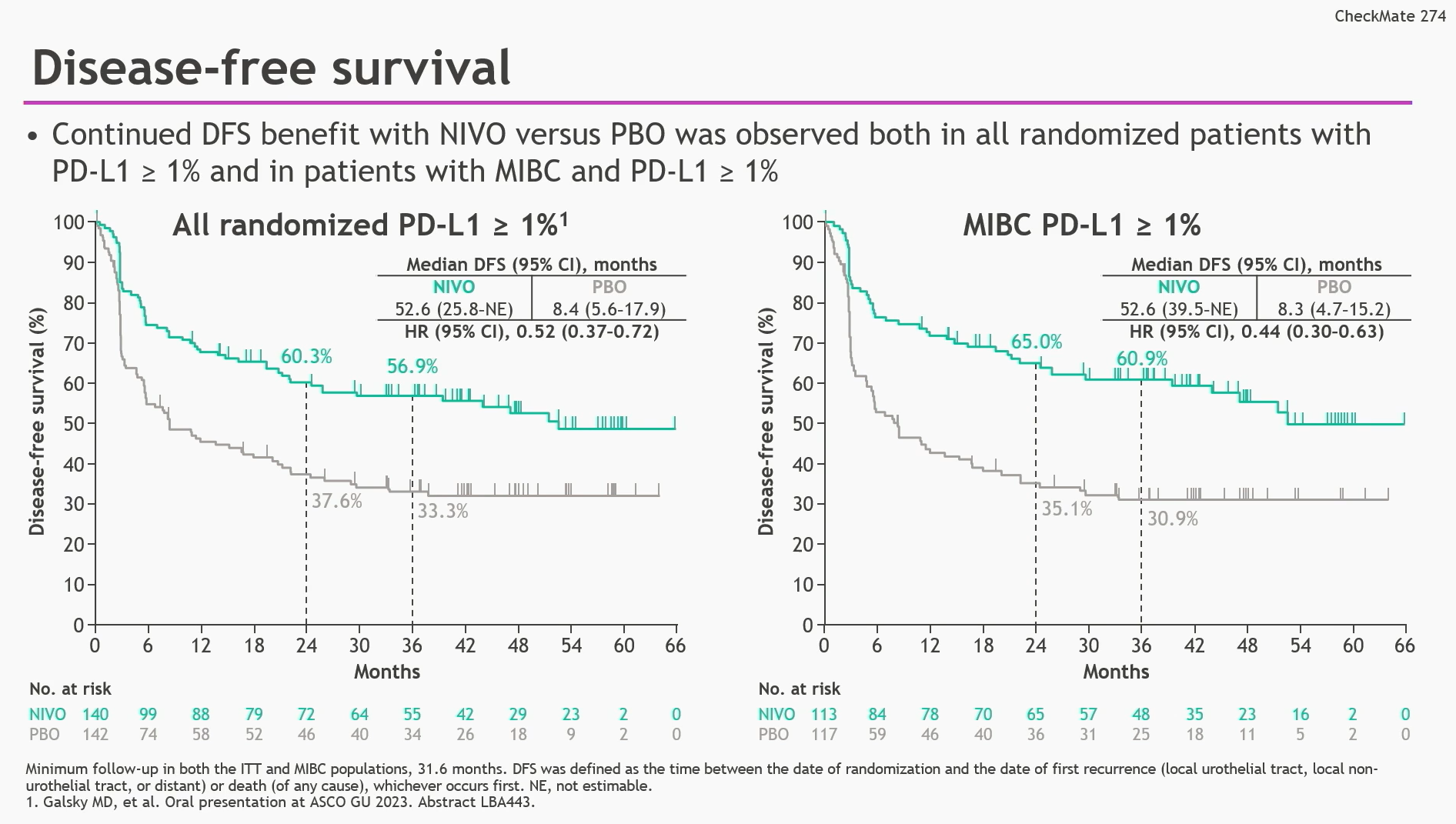
Specifically, the median DFS achieved with adjuvant nivolumab in the intent-to-treat (ITT) population was 21.0 months vs 10.9 months with placebo (HR, 0.70 98.31% CI, 0.54-0.89 P <.001). The application is based on data from the phase 3 CheckMate-274 trial (NCT02632409), which showed that when nivolumab was given after surgery, patients with MIUC experienced an improvement in disease-free survival (DFS). The European Medicines Agency has validated its type II variation application for nivolumab (Opdivo) as an adjuvant treatment for patients with surgically resected, high-risk muscle-invasive urothelial carcinoma (MIUC), according to an announcement from Bristol Myers Squibb. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
